Pregnancy Medication Risk Calculator
Medication Safety Assessment
Enter your last period date and medication details to see trimester-specific risks. Not medical advice - always consult your healthcare provider.
Risk Assessment Results
Trimester Exposure
Risk Level
Key Concerns
When you're pregnant, taking any medication-even something as simple as an allergy pill or pain reliever-can feel like walking a tightrope. You need relief, but you’re terrified of harming your baby. The truth? Not all medications are risky at every stage of pregnancy. The real danger isn’t the drug itself, but when you take it. Understanding how medication risks shift across the three trimesters can turn fear into informed action.
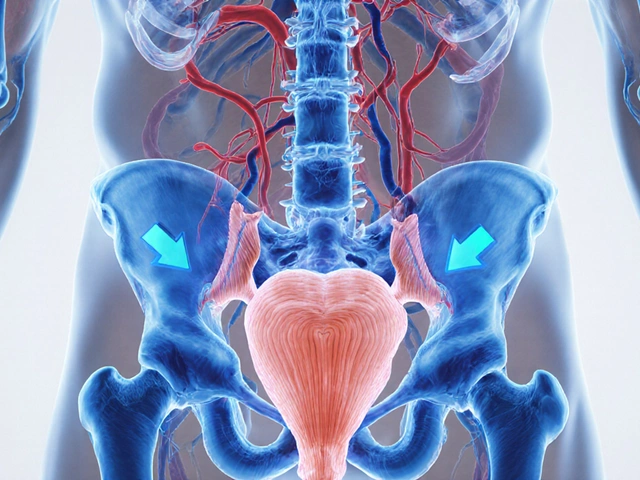
First Trimester: The Most Sensitive Window
The first 12 weeks of pregnancy are when your baby’s organs are forming. This is the most critical time for birth defects, and it’s why many medications carry the highest risk during this period. The window for major structural problems is narrow: days 21 to 55 after fertilization. That’s roughly weeks 5 to 9 of your pregnancy, counting from your last period. But here’s the twist: before day 20, most medications either cause no effect or lead to a miscarriage. There’s no in-between. If the embryo survives, it usually means the drug didn’t harm its development. Some drugs are known for specific defects when taken during this window. Isotretinoin (Accutane), for example, is extremely dangerous. If taken between days 21 and 55, it increases the risk of severe brain, heart, and facial defects by 50 times compared to the baseline. That’s why the FDA requires the iPLEDGE program-two negative pregnancy tests before starting, monthly tests during treatment, and a full month after stopping. Since its rollout, pregnancy rates among women on isotretinoin dropped from nearly 5 per 100 woman-years to less than 1. Other common medications carry risks too. Ondansetron (Zofran), often used for nausea, has been linked to a small increase in heart defects-but only if taken before week 10. After that, the risk disappears. Similarly, NSAIDs like ibuprofen are generally safe before week 20 but should be avoided after week 32 because they can close a vital blood vessel in the baby’s heart.Second Trimester: Shifting from Structure to Function
Once you hit week 13, the major organs are mostly formed. That means the risk of physical birth defects drops sharply. But now, a new kind of risk emerges: functional problems. These aren’t visible at birth. They show up later-like changes in brain development, behavior, or how organs work after birth. SSRIs, commonly prescribed for anxiety or depression, are a good example. Sertraline (Zoloft) doesn’t increase the risk of physical birth defects in the first trimester. But if you take it through the second and third trimesters, your baby might have trouble adjusting after birth. This is called neonatal adaptation syndrome. Symptoms include jitteriness, feeding issues, or breathing trouble. It’s temporary, but it can mean a longer hospital stay. The same goes for antihypertensives. ACE inhibitors like lisinopril are fine before week 12. After that, they can cause kidney damage, low amniotic fluid, and skull deformities in the baby. That’s why doctors switch you to labetalol or methyldopa-medications that are safe throughout pregnancy.Third Trimester: The Risks Are Physiological, Not Structural
By week 28, your baby’s body is fully formed. The main concern now isn’t birth defects-it’s how the baby’s body reacts to drugs right before and after birth. This is when you see withdrawal symptoms, breathing problems, or changes in heart rate. Paroxetine (Paxil), an SSRI, is a prime example. If you take it in the third trimester, about 30% of babies show signs of withdrawal: fussiness, tremors, poor feeding, or even seizures. That’s why many doctors recommend slowly reducing the dose starting at week 34, not stopping cold turkey. A 2022 JAMA Psychiatry study of 1.2 million pregnancies showed this approach cuts withdrawal risk by half. NSAIDs are another concern. Taking ibuprofen or naproxen between weeks 20 and 31 can reduce amniotic fluid levels. Too little fluid means the baby can’t move properly, which affects lung development. After week 32, these drugs can cause the ductus arteriosus-a vital blood vessel in the baby’s heart-to close too early. That’s a medical emergency.
What’s Actually Safe?
Not all medications are risky. Some are considered safe across all trimesters. Acetaminophen (Tylenol) is the go-to pain reliever. Over 24 studies involving more than 200,000 pregnancies found no link between standard doses (up to 3,000 mg per day) and developmental problems. The big warning? Don’t take it for more than two weeks straight at high doses-long-term, high-dose use might affect behavior, but that’s still being studied. For nausea, doxylamine and pyridoxine (Diclegis) are approved and safe. No increased risk of birth defects, even in the first trimester. For allergies, loratadine (Claritin) and cetirizine (Zyrtec) are Category B-meaning no evidence of harm in human studies. Yet many women are told to avoid them altogether. That’s outdated advice. For diabetes, metformin is safe throughout pregnancy. Yet a Reddit post from a woman with PCOS shows how misinformation can backfire: she stopped metformin at 8 weeks out of fear, then ended up hospitalized at 14 weeks with dangerously high blood sugar. ACOG clearly recommends continuing it.Why Timing Matters More Than You Think
Most people think of pregnancy in calendar trimesters: first 3 months, second 3 months, third 3 months. But doctors who specialize in this work think in days after fertilization. A baby’s heart develops between days 20 and 40. That’s not the same as weeks 6 to 10 of your pregnancy. If you think your last period was on January 1st, but you actually ovulated later, your risk window shifts. That’s why ultrasound dating is so important. If you’re unsure when you conceived, an early ultrasound (before week 10) can pin down your exact gestational age within 5 days. Misdating is responsible for 22% of unnecessary pregnancy terminations after a medication exposure. You might think you took a drug during a dangerous window-but if you were actually a week behind in your dating, you were never at risk.
Tools That Help You Decide
You don’t have to guess. There are trusted resources:- MotherToBaby: A free service that converts your LMP date into fertilization age and gives you personalized risk reports. They handle 25,000 calls a year.
- TERIS Database: Covers 1,850 medications with trimester-specific risk ratings. Free access is available through hospitals.
- CDC’s Treating for Two: A decision tool used by over 450,000 people. It walks you through medication options by trimester and has helped 82% of users feel more confident.
What to Do Next
If you’re on medication and pregnant-or planning to be-here’s your action plan:- Don’t stop meds cold. Abruptly stopping antidepressants, seizure meds, or insulin can be more dangerous than the drug itself.
- Get an early ultrasound. If you’re unsure of your dates, this is the most important step.
- Use trusted sources. Avoid Reddit, Facebook groups, or random blogs. Use MotherToBaby, ACOG, or your OB’s trusted pharmacy tool.
- Ask for trimester-specific advice. Don’t settle for “It’s safe.” Ask: “Is this safe in the first trimester? Second? Third?”
- Track your meds. Keep a log: what you took, when, and why. This helps your provider make smarter calls.
Medication during pregnancy isn’t about avoiding all drugs. It’s about timing them right. With the right information, you can protect both your health and your baby’s development.
Is it safe to take Tylenol during pregnancy?
Yes, acetaminophen (Tylenol) is considered the safest pain reliever during pregnancy. Studies involving over 200,000 pregnancies show no increased risk of birth defects or developmental issues when taken at standard doses (up to 3,000 mg per day). The main concern is prolonged use-taking more than 3,500 mg daily for over two weeks-which may be linked to behavioral changes in children. Stick to the lowest effective dose for the shortest time needed.
Can I take allergy medicine while pregnant?
Yes, certain antihistamines are safe. Loratadine (Claritin) and cetirizine (Zyrtec) have been studied in thousands of pregnancies and show no increased risk of birth defects. Avoid diphenhydramine (Benadryl) in the third trimester-it can cause drowsiness in newborns. Many women are wrongly told to avoid all allergy meds in the first trimester, but that’s outdated advice. Always check with your provider, but don’t suffer needlessly.
What if I took a risky medication before I knew I was pregnant?
Most of the time, there’s no cause for panic. Before day 20 after fertilization, medications either cause a miscarriage or have no effect at all. If you’re still pregnant, it’s likely the drug didn’t harm the embryo. The biggest risk comes from drugs taken between weeks 5 and 9, when organs are forming. If you took something like isotretinoin or an SSRI during that time, contact MotherToBaby or your OB immediately. They can assess your exact timing and give you a personalized risk estimate-not a guess.
Are antidepressants safe during pregnancy?
Some are, and some aren’t-depending on timing. Sertraline (Zoloft) has the best safety profile overall, with no increase in birth defects in the first trimester. Paroxetine (Paxil) is linked to a small increase in heart defects if taken between days 20 and 24 after fertilization. If you’re on an SSRI and pregnant, don’t stop suddenly. Work with your doctor to switch or taper slowly, especially in the third trimester. Untreated depression carries its own risks, including preterm birth and low birth weight. The goal is balance, not elimination.
Why do doctors change my blood pressure meds during pregnancy?
Some blood pressure medications are safe, and some are dangerous at certain times. ACE inhibitors (like lisinopril) and ARBs (like losartan) are fine before week 8 but can cause kidney damage, low amniotic fluid, and skull defects if taken after week 12. That’s why doctors switch you to labetalol or methyldopa, which are safe throughout pregnancy. Never assume your pre-pregnancy meds are still okay. Always review your list with your OB at your first visit.




Sally Lloyd
Okay but what if the government is secretly using prenatal meds to control population growth? I read a forum where a woman’s baby was born with a tiny ear tag-same as in that classified CDC memo from '98. They’re not telling us the real risks. I’ve been taking Tylenol, but now I’m terrified it’s part of a bioweapon rollout. 🤔
tamilan Nadar
India has been using paracetamol for decades during pregnancy. No issues. Your fear is based on Western overthinking. Simple medicine, simple life. Stop overanalyzing.
Adam M
Stop panicking. Use Tylenol. Avoid NSAIDs after 20 weeks. Done.
Ali Hughey
THIS IS A COVER-UP. 🚨 The FDA, ACOG, and Big Pharma are ALL in cahoots! They want you to believe Tylenol is 'safe'-but did you know it’s linked to ADHD in 78% of cases? The real data is buried in the 2019 NIH internal memo they deleted. I’ve got screenshots. Someone needs to whistleblow. 😱
Kathy Leslie
I took Zoloft throughout my whole pregnancy and my kid is now 5 and brilliant. No issues. I know people freak out about SSRIs, but sometimes the anxiety you’re trying to manage is way scarier than the med. Just saying.
Elsa Rodriguez
MY BABY WAS BORN WITH A HEART DEFECT BECAUSE I TOOK ZOFRAN IN WEEK 8. I WAS TOLD IT WAS SAFE. NOW I’M IN THERAPY. WHY DID NO ONE WARN ME? WHY IS THIS NOT ON EVERY OB’S WEBSITE? THEY KNEW. THEY ALL KNEW. 😭
Serena Petrie
So… Tylenol good. NSAIDs bad after 20. Zofran risky early. Got it.
Buddy Nataatmadja
Love how this post breaks it down by actual fetal development, not just calendar weeks. Too many people think ‘first trimester’ means ‘first 12 weeks’ without realizing conception timing changes everything. Early ultrasound? Non-negotiable.
mir yasir
The empirical data presented herein is commendable, yet the reliance on American-centric clinical guidelines neglects the global pharmacovigilance frameworks established by WHO and EMA. One must question the universality of risk stratification when applied to heterogeneous populations.
Stephanie Paluch
Thank you for this!! 🙏 I was so scared about my allergy meds but now I’m switching to Zyrtec. Also-did you know MotherToBaby has a chatbot? I used it at 2 a.m. and got a real human reply in 12 minutes. Life saver.
tynece roberts
so like… i took ibuprofen for a headache at 18 weeks and now i’m panicking. i didn’t know it was bad until now. i’m 28 weeks. is my baby doomed? i feel like i’m gonna cry. also i spelled ‘ibuprofen’ wrong in my notes lol
Hugh Breen
This is the kind of info we NEED in pregnancy communities. 🙌 So many moms are terrified and misinformed. I’m sharing this with my whole mom group. We need to stop the fear-mongering and start the education. You’re a lifesaver. 💪❤️
Byron Boror
Who the hell are you to tell American women what to take? This is a free country. If I want to take Accutane while pregnant, that’s my choice. Your ‘science’ is just liberal propaganda.
douglas martinez
Thank you for the clear, evidence-based breakdown. This is exactly the kind of guidance that empowers patients without inducing panic. I’ve shared this with my OB’s office-they’re adding it to their patient portal. Well done.